|
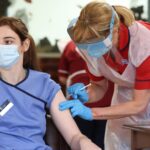
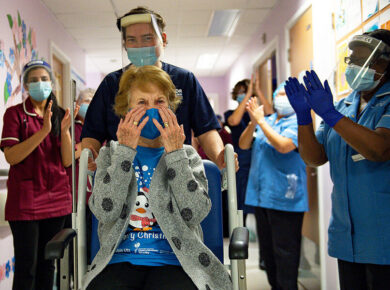
As Vaccines Roll Out, States Face Difficult Questions Over Access11 Dec 2020
Charlotte Evans is avidly watching the news about coronavirus vaccines – and as soon as one is available to her,... Continue Reading
|

|
HHS Floats Major Changes to HIPAA Privacy Rule11 Dec 2020
The new proposed rule would “break down barriers that have stood in the way of commonsense care coordination and value-based... Continue Reading
|

|
ATA Responds to CMS Final Rule Making Some Telehealth Coverage Permanent11 Dec 2020
Although the American Telemedicine Association commended the agency’s moves to expand some services, it urged CMS to reconsider its approach... Continue Reading
|

|
Mayo Clinic CIO says AI has Been Key to Understanding COVID-1911 Dec 2020
From genetic sequencing to symptom tracking to vaccine development, machine learning algorithms have been instrumental in helping uncover hidden clues... Continue Reading
|

|
Telehealth, Vaccines Will be Big Cybersecurity Challenges in 2021, Experts Predict11 Dec 2020
The latest security industry forecast from Experian warns that bad actors will continue to take advantage of the COVID-19 crisis... Continue Reading
|
|
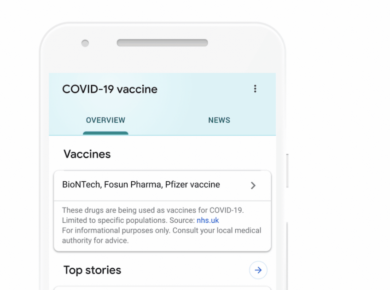
Google Takes on COVID-19 Vaccine Misinformation11 Dec 2020
The tech giant is adding new searches for COVID-19 vaccines, new funds for fact-checking initiatives and efforts to remove misleading... Continue Reading
|

|
How Google, Facebook and Apple Tools are Fueling COVID-19 Disinformation Sites11 Dec 2020
Tech companies including Facebook, Google and Apple that are working to prevent COVID-19 disinformation and fraud on their platforms are... Continue Reading
|

|
HIMSS CEO: How to Capitalize on An ‘Exponential Growth’ in Digital Innovation04 Nov 2020
The COVID-19 crisis has led to major leaps forward for telehealth, decision support and more, says Hal Wolf – but... Continue Reading
|

|
AMA: 4 Ways Providers can Use Social Media to Improve Public Health04 Nov 2020
The COVID-19 pandemic has shined a light on the power of social media in healthcare and its ability to quickly... Continue Reading
|

|
Mayo Clinic, Google Announce Ai Effort to Boost Radiation Therapy for Cancer04 Nov 2020
Mayo Clinic and Google Health have announced they will use artificial intelligence to improve radiation therapy planning for cancer care.... Continue Reading
|