In a bid to overcome the state legislature’s reticence to pass Medicaid expansion, citizens of Utah made it a referendum issue; in November 2018, voters passed Proposition 3 to expand the program. However, Utah has just enacted a law that would significantly alter the voter-approved measure. Instead of pursuing a conventional expansion, the bill signed by the governor on Monday proposes a limited “partial expansion” of eligibility funded at the standard, lower federal matching rate of 68 percent with a fallback position of a full expansion with additional waiver requirements. Utah will then ask the Centers for Medicare and Medicaid Services (CMS) to increase the matching financing rate to the enhanced federal share of 90 percent.
Other states, such as Tennessee and Georgia are closely observing Utah’s actions as a potential template for similar, partial expansions of Medicaid.
Why Partial Expansion?
The impetus for partial expansion grows out of complicated—and conflicting—eligibility rules for Medicaid and federal financial assistance to purchase private coverage on state insurance marketplaces. The Affordable Care Act (ACA) provided for Medicaid expansion up to 138 percent of the federal poverty level (FPL), but initiated eligibility for tax credits at 100 percent FPL; reporting suggests that this was a legislative drafting oversight. Since the ACA’s implementation, it has been understood that households eligible for Medicaid enrollment do not additionally qualify for federal tax credits; people between 100 and 138 percent FPL have only received tax credits in states which did not elect to expand Medicaid. Under President Obama, CMS released guidance stating that partially expanding Medicaid up to 100 percent FPL was not permissible under the text of the law; it remains to be seen whether the agency will abide by that principle under current leadership.
Proposition 3, which passed with 53 percent public support, fully expanded eligibility to 138 percent FPL, with an operational start date of April 1, 2019. Provider reimbursement and eligibility and enrollment standards were to be maintained to the standards used on January 1, 2017. Voters approved an increase in the state sales tax to fund the state share of Medicaid expansion. Measures that might actively inhibit enrollment, like work requirements and enrollment caps, were not part of the proposition.
Want to publish your own articles on DistilINFO Publications?
Send us an email, we will get in touch with you.
The legislature’s bill represents a significant deviation from the ballot measure described above. It proposes a partial expansion, restricting eligibility to individuals earning less than 100 percent FPL. The bill goes farther than limiting the expansion population, though. Work requirements and enrollment caps would be included. Federal funding would come from a per capita block grant. Per capita grants are designed to lower federal costs by offering states increased flexibility from rules while eliminating the individual entitlement to Medicaid and placing the entire onus of unexpected costs on state budgets.
This proposal has significant local and national policy implications.
On-Exchange Implications Of A Limited Medicaid Expansion
Because those Utahans between 100 and 138 percent FPL are already eligible for subsidized enrollment on the state insurance exchange, a partial expansion increasing Medicaid eligibility up to the poverty line would not change current on-exchange pricing dynamics. However, it is important to evaluate the potential impacts of a partial expansion against the counterfactual of a full expansion. This analysis must take into account the evolving nature of the Affordable Care Act due to regulatory actions by the Trump administration.
Previous evidence found that Medicaid expansion improved the risk pool of state individual markets, suggesting that the population between 100 and 138 percent FPL is sicker and more expensive, on average, than other exchange enrollees. Insuring this cohort through Medicaid is associated with a seven to eleven percentage point decrease in individual market premiums. These analyses were performed during a time when cost-sharing reductions (CSRs, which are supplemental subsidies available to exchange enrollees below 250 percent FPL) were fully funded. The Trump administration announced that they would halt this funding in October 2017.
However, insurers were still legally obligated to provide the financial protections that these subsidies offered; the termination of federal CSR payments led insurers in nearly all states to incorporate these costs into their premiums. In 2019 and beyond, all states responded to CSR termination by either “silver loading” (placing the incremental cost of CSRs onto only silver plans) or “broad loading” (distributing the incremental cost across metal tiers). Silver loading elevates the benchmark premium faster than bronze and gold plan premiums. Because tax credits are calculated based on the benchmark premium, this leads to larger subsidies and better non-silver pricing for subsidized buyers. Silver loading has been the dominant reaction.
Medicaid expansion and these CSR strategies interact in complex ways, with important implications for enrollees. CSRs help offset out-of-pocket health costs like deductibles and copays, improving the actuarial value (AV) of the plan. However, enrollees can only access CSRs if they enroll in a silver plan; the supplemental assistance is not available on the bronze or gold tiers. There are three levels of CSR generosity, depending on income. For people between 100 percent and 150 percent FPL, CSRs bring the AV of a silver plan from 70 percent to 94 percent. For people between 150 percent and 200 percent FPL, the supplemental subsidies result in 87 percent AV silver plans, and for those between 200 and 250 percent FPL, the actuarial value is a more modest 73 percent. For reference, plans in the gold tier have actuarial values of 80 percent.
When considering partial expansion, we are particularly concerned about those with household incomes between 100 percent and 150 percent FPL, those that would be eligible for 94 percent AV silver plans. This income bracket overlaps the Medicaid expansion income group significantly. States that fully expand Medicaid end up with far fewer people in the most generous CSR bucket, as they have moved the 100-138 percent population to Medicaid (see Exhibit 1).
Exhibit 1: 2018 Enrollment In CSR 94 plans As Percentage Of APTC Population
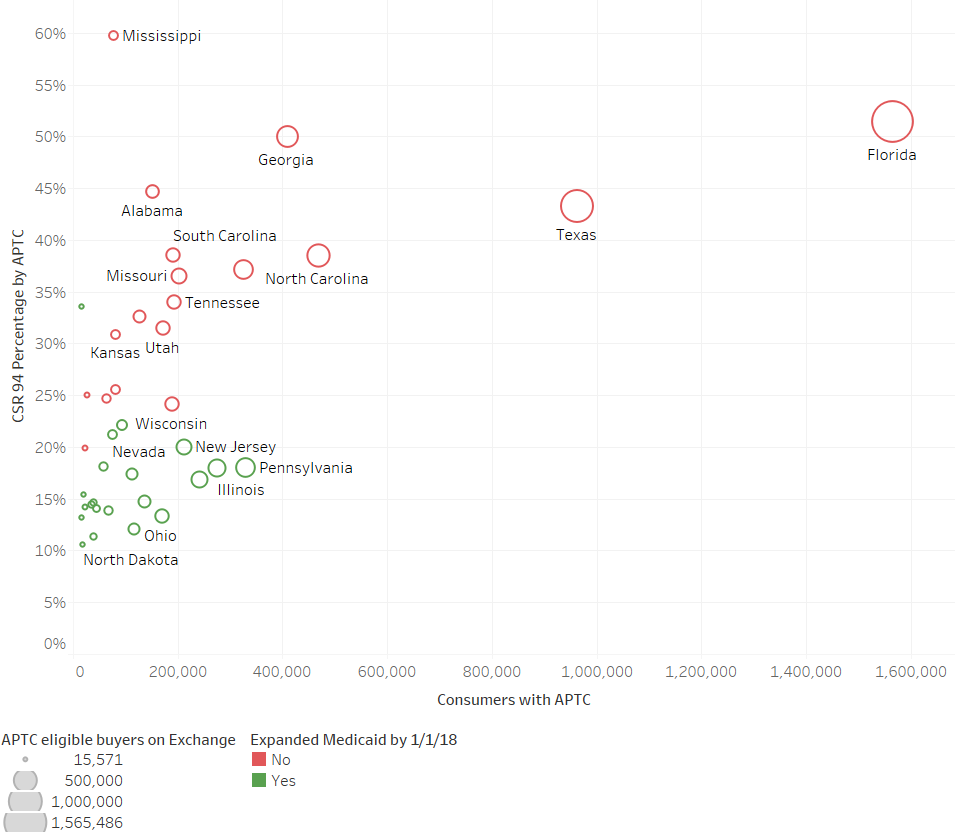
Sources: Author Calculations
2018 Open Enrollment PUF State Level Public Use File Tab 5 By Premium and FA
https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/Marketplace-Products/2018_Open_Enrollment.html
Kaiser Family Foundation Medicaid Expansion Tracker used to mark states as Expansion/NonExpansion as of 1/1/18
https://www.kff.org/health-reform/state-indicator/state-activity-around-expanding-medicaid-under-the-affordable-care-act/
Percentage of total on-exchange enrollees with 94 percent AV CSR Plan divided by total enrollees with APTC
Silver loading is, perhaps unexpectedly, a more powerful tool for affordability in states that haven’t expanded Medicaid; that marginally sicker would-be-Medicaid population between 100 and 138 percent FPL drives up premiums for benchmark plans—and the subsidies that are calculated off of those benchmarks. In states using Healthcare.gov, those that had expanded Medicaid lost more enrollment than non-expansion states after federal CSR payments were terminated.
This pricing policy predominantly benefits individual market buyers who make between 200 percent and 400 percent of the federal poverty level because this population qualifies for weak (73 percent AV) or no supplemental assistance—but they benefit from relatively lower bronze and gold premiums.
These silver-loaded policies only benefit those exchange enrollees who qualify for federal tax credits. The proposal by Utah’s legislature succeeds in expanding Medicaid to only 100 percent of the federal poverty line, keeping the 100-138 percent FPL cohort in the exchange means a sicker risk pool with higher premiums for unsubsidized enrollees, relative to a world where the state fully expands the program to 138 percent FPL.
Tradeoffs Between Medicaid Coverage And Private Plans
How these policy decisions play out for households earning between 100 to 138 percent of the federal poverty level depends on healthcare utilization. A 40 year old individual earning $13,000 in 2019 can buy a 94 percent AV silver plan for $5 per month or 0.35 percent of income as there is a modest gap in premium between the benchmark silver and the least expensive silver plan. Other states’ waivers have allowed for premiums of two percent of income to be charged. Individuals with low to no utilization who are price sensitive and network indifferent are better off on the Exchange when there is a modest little difference in premiums between the least expensive silver plan and the benchmark silver plan.
These are some of the market trade-offs that must be considered if a state wishes to pursue a partial Medicaid expansion. But there are also tradeoffs for the beneficiaries who would be most directly affected by Utah fully expanding—those Utahans who would be moved into Medicaid.
As discussed above, Medicaid provides more financial protection for beneficiaries. It has stricter limits on out-of-pocket expenditures, making it more generous even than highly subsidized silver plans. Medicaid limits out of pocket costs to no more than five percent of income while silver plans with CSRs applied have cost sharing limits of ten percent or more of a qualified individual’s income.
There are other protections and benefits inherent to Medicaid that enrollees aren’t likely to receive in private health plans. For example, Medicaid offers non-emergency medical transportation, to assist beneficiaries in getting to their medical appointments. Unlike exchange plans, Medicaid does not have a dedicated open enrollment period; people can enroll at any time. Furthermore, the program has retroactive coverage provisions—coverage can be backdated up to 3 months upon enrollment, if the individual was eligible for the program during those months. Some states, however, have been seeking permission from the federal government to scale back this retroactive coverage (indeed, Utah has waived retroactive eligibility for some people currently eligible for Medicaid in the state). Retroactive coverage measures offer a protective effect for Medicaid-eligible individuals who are unaware that they qualify for the program; polling suggests that poor understanding of eligibility for public insurance and federal subsidies may be one reason that coverage gains haven’t been more widespread.
Furthermore, subsidizing individuals to enroll in private plans is more expensive than covering those same people on Medicaid. States are likely to find the more expensive option attractive, because they do not directly bear the burden of paying the federal tax credits that make these plans affordable for lower-income households. By contrast, Utah would be responsible for shouldering 10 percent of the cost of the Medicaid expansion population from 2020 forward. Partial expansion is thus a clear winner from the state budgeter’s perspective, but a potential loser for the federal government—partial expansion is only a less expensive proposition if fewer people enroll in coverage. A higher-than-necessary uninsured population is a plausible outcome under partial expansion, but hardly a desirable one when considering policy strategies to encourage better health at lower costs.
Final Thoughts
The considerations above mostly favor a broader Medicaid expansion, when considering the perspective of someone who would shift from private coverage to the state program. However, that transition would inevitably be disruptive for some people with established care relationships. As with any insurance transition—private plan to private plan, or private plan to Medicaid—there is no guarantee that a person’s providers will accept the new form of coverage.
These tradeoffs are worth consideration, but so is the dyspeptic political landscape in which they are set to play out. Partial expansion, as a theoretical proposition, has become a subject of scrutiny and debate. Some argue that such expansions are superior to no expansion at all, so permitting states to bring only those below the poverty line into the Medicaid fold is a tolerable compromise.
However, that is not the scenario that Utah is confronting at the moment. The state’s voters passed a referendum to implement a full expansion; the new law represents a pernicious effort to override the will of that popular vote.
Date: February 20, 2019
Source: Health Affairs







